Over the past decade, rates of mental illness, drug overdoses, and suicides have risen sharply across the United States, signaling a growing crisis in behavioral health. According to the Centers for Disease Control and Prevention (CDC), the prevalence of depression and anxiety disorders has increased significantly, with young adults and historically underserved communities experiencing some of the steepest rises. At the same time, the country has witnessed record-breaking numbers of drug overdose deaths, largely driven by opioids and synthetic substances like fentanyl. Suicide rates have also climbed, particularly among adolescents, veterans, and rural populations, underscoring the urgent need for accessible mental health care.
Despite this growing demand, many communities face a severe shortage of mental health professionals such as psychologists, counselors, therapists, social workers, and psychiatrists, among others. To assess where these shortages are most acute, Addiction-Rep—a consulting firm for rehab and addiction treatment centers—analyzed data from multiple federal sources, measuring the number of mental health professionals per 10,000 residents in the nation’s 100 largest metropolitan areas and all 50 states. The findings highlight significant disparities in mental health workforce availability, particularly in the South and pockets of the Mountain West.
Rates of Mental Illness in the United States
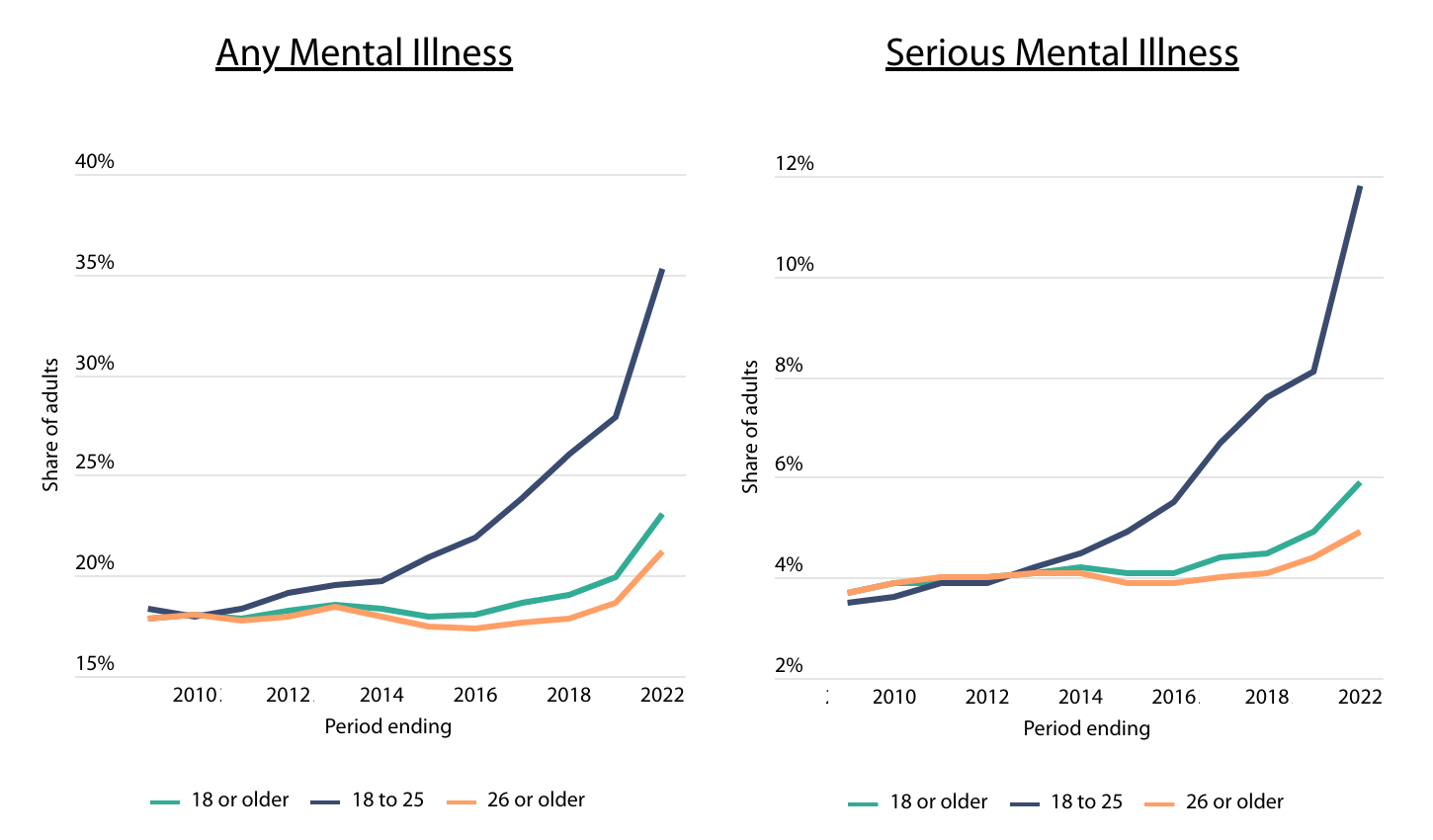
Source: Addiction-Rep analysis of SAMHSA data | Image Credit: Addiction-Rep
Mental illness has become increasingly prevalent in the U.S. in recent years, with particularly sharp increases among young adults. According to data from the Substance Abuse and Mental Health Services Administration (SAMHSA), the percentage of U.S. adults reporting any mental illness (AMI) in the past year rose from 17.9% in 2009 to 23.1% in 2022. However, this increase has been far more pronounced among individuals aged 18 to 25, where rates jumped from 18.3% in 2009 to 35.3% in 2022—nearly doubling over this period. In contrast, the prevalence of mental illness among adults 26 and older increased more gradually, from 17.9% in 2009 to 21.2% in 2022.
More severe forms of mental illness, categorized as serious mental illness (SMI), have also become more common. SMIs are defined as mental health conditions that substantially interfere with a person’s ability to function, including disorders such as bipolar disorder, major depressive disorder, and schizophrenia. The data shows that while overall rates of SMI rose from 3.7% in 2009 to 5.9% in 2022, young adults again saw the most dramatic increase. Among those aged 18 to 25, the rate of SMI more than tripled, rising from 3.5% in 2009 to 11.8% in 2022. Meanwhile, SMI prevalence among those 26 and older grew at a slower pace, from 3.7% to 4.9% over the same period.
The Growing Shortage of Mental Health Workers

Source: Addiction-Rep analysis of HRSA data | Image Credit: Addiction-Rep
Amid rising rates of mental illness, the U.S. is facing a severe shortage of mental health professionals, making it increasingly difficult for individuals to access care. Many behavioral health roles are affected, with shortages driven by an aging workforce, low wages, and high burnout rates. Without intervention, the gap between available professionals and those in need of care is expected to widen significantly in the coming years.
Two critical examples of this shortage are addiction counselors and mental health counselors. According to Health Resources and Services Administration (HRSA) projections, the demand for addiction counselors will grow from 129,250 in 2022 to over 206,000 by 2037, while supply is expected to shrink to just 92,160, creating a shortfall of nearly 114,000 professionals. Similarly, the demand for mental health counselors is projected to rise from 128,600 in 2022 to 203,140 by 2037, while the available workforce is projected to decline. This imbalance will result in a shortage of almost 88,000 counselors, further straining access to mental health care.
Mental Health Worker Shortages by State & Metro

Source: Addiction-Rep analysis of BLS and ACS data | Image Credit: Addiction-Rep
While the gap in mental health services is expected to widen in the coming years, some states are already experiencing severe shortages. Nationwide, there are 58.3 mental health workers per 10,000 residents, but several states, particularly in the South and Southwest, fall far below this average. Georgia (36.4), Alabama (38.8), Texas (40.0), and Arkansas (40.3) have the lowest mental health workforce per capita, highlighting a critical gap in services. In contrast, Massachusetts (96.9), Vermont (84.7), and Rhode Island (73.8) have some of the highest numbers, reinforcing a regional divide where the Northeast generally has better access to mental health providers compared to the South and West.
At the metropolitan level, cities in Florida, Texas, and the Southeast have the most severe shortages. Fayetteville, AR (27.4), Huntsville, AL (27.6), and Lakeland, FL (28.6) rank among the lowest, while larger metros like Atlanta (36.4), Dallas (36.6), and Houston (36.9) also fall well below the national average. At the opposite end of the spectrum, some cities—particularly in the Northeast, Midwest, and West Coast—have far greater access to mental health professionals. Springfield, MA (112.5), Madison, WI (93.4), and Boston (92.3) lead the nation, mirroring state-level trends. Several California metros rank well, including Los Angeles (85.4), San Diego (76.1), and San Francisco (74.9).
As demand for behavioral health services continues to rise, regions already struggling with shortages will face even greater challenges in the years ahead. Without significant policy interventions, such as increased funding for mental health programs and expanded training pipelines, the gap between supply and demand is likely to worsen—leaving millions without the care they need.
Methodology

Photo Credit: Pormezz / Shutterstock
This analysis identifies metropolitan areas with the largest shortages of mental health workers using data from multiple authoritative sources, including the U.S. Bureau of Labor Statistics (BLS) Occupational Employment and Wage Statistics (OEWS), U.S. Census Bureau American Community Survey (ACS), Centers for Disease Control and Prevention (CDC) Behavioral Risk Factor Surveillance System (BRFSS), Substance Abuse and Mental Health Services Administration (SAMHSA) National Survey on Drug Use and Health (NSDUH), and Health Resources and Services Administration (HRSA) Workforce Projections.
To measure mental health workforce shortages, researchers at Addiction-Rep calculated the number of mental health professionals per 10,000 residents across major metropolitan statistical areas (MSAs) and states. For this study, mental health professionals were defined as individuals employed in the following occupations: Clinical and Counseling Psychologists; School Psychologists; Psychologists, All Other; Educational, Guidance, and Career Counselors and Advisors; Marriage and Family Therapists; Rehabilitation Counselors; Substance Abuse, Behavioral Disorder, and Mental Health Counselors; Counselors, All Other; Child, Family, and School Social Workers; Healthcare Social Workers; Mental Health and Substance Abuse Social Workers; Social Workers, All Other; Psychiatrists; Psychiatric Technicians; and Psychiatric Aides.
Mental health statistics reflect the adult population (ages 18 and over). The CDC defines the prevalence of depression as the percentage of individuals who have ever been diagnosed with a depressive disorder. The prevalence of frequent mental distress is determined by the percentage of respondents who reported experiencing poor mental health on at least 14 of the past 30 days.
To ensure consistency and accuracy, only metropolitan areas with complete data from all sources were included. Given variations in data collection periods, the presented statistics span 2022–2023, depending on geography and dataset availability. Additionally, to enhance the reliability of the metro-level estimates, only the 100 largest MSAs (by total employment) were analyzed.
For complete results, see Cities With the Largest Shortage of Mental Health Workers on Addiction-Rep.